I saw an article that gave me some hope for our current bacterial and viral dilemmas; it involved a new strategy to prevent infections, rather than treating them after they've struck. I'm all for preventive medicine, both in the infectious disease arena and in medicine in general. I think we "play catch-up" all too often.
The piece was in The Wall Street Journal on May 30, 21013 with its headline, "New Tack in Preventing Hospital Infections: Germ-Killing Soap-Ointment Treatment for all ICU Patients Shown to be More Effective than Isolating Some After Screening" The original article was printed online in the New England Journal of Medicine on May 29, 2013 and its title was "Targeted versus Universal Decolonization to Prevent ICU Infection."
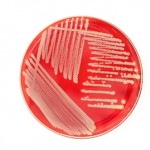
We're mostly talking about MRSA (Methicillin-resistant Staphylococcus aureus), that strain of the familiar Staph bacteria that's been plaguing us for the last few decades, in large part as a result of unnecessary antibiotic use.
Even if antibiotics are used only for significant bacterial infections, a small proportion of the "bugs" may survive. The population of those germs who cannot be killed by the particular antibiotic can multiply and be spread to others. When antimicrobial drugs are used inappropriately used to "treat" viral infections (e.g., "flu" or the common cold) or given wholesale to food animals (beef, chicken, pigs) to promote growth), we're also likely to be find ourselves with bacteria that are resistant to those antibiotics we've previously been able to use successfully.
About 30% of us carry staph of our skin or in our nostrils (without being ill) and somewhere between 1% and 2.5% carry MRSA. Otherwise healthy people can develop infection with it as a painful skin boil, especially in rugby or football players and high school wrestlers, but also in those who are child care workers or live in crowded settings.
Since moving here in 1999 I'm personally aware of two people who started with what seemed to be very minor skin infections, but later were diagnosed with extremely serious progression of their initial disease. One died from what was eventually diagnosed as fleshing-eating Strep; the other survived, but spend a long time in intensive care with a Staph infection that spread from a bump on his arm up to his chest.
Hospitals often screen patients for MRSA and nine states now mandate such screening. But the study mentioned above attempted to see if there was a better way to avert serious infections in the intensive care setting where patients are the sickest.
Forty-three hospitals with 74 ICUs and nearly 75,000 patents were randomly assigned to one of three infection prevention strategies: the first group screened patents for MRSA and isolated those who tested positive; the second group added "decolonization," removing the bacteria by washing MRSA-positive patents with an antimicrobial (bacteria-killing) soap plus giving them a nasal antibiotic; the third group of hospitals did not screen patents, but treated every ICU patient as though they had MRSA, i.e., with the soap and the nasal antibiotic.
Universal decolonization cut the rate of positive blood cultures, a way to look at the most serious infections, by 44%. That included not only Staph, but other bacteria as well. Only seven of the research subjects had any form of adverse reaction and those were mild rashes of itching; all resolved after stopping the washing.
The Mayo Clinic webpage on MRSA discusses risk factors for hospital-associated MRSA infections (HA-MRSA) and for those that are community-associated (CA-MRSA). Just being hospitalized increases your risk as does having an invasive medical device (urinary catheter or IV line) and residing in a long-term care facility. Remember, carriers of MRSA can spread the germ, even if they are not sick from it. For CA-MRSA the risk factors include contact sport, living in crowded or unsanitary conditions and men who have homosexual relations.
The World Health Organization (WHO) has an online fact sheet on Antimicrobial resistance. Infections that fail to respond to conventional therapy result in higher medical care costs, greater length of illnesses and a higher risk of a fatal outcome.
MRSA is by no means the only germ that has developed drug resistance. WHO estimates over 630,000 cases of multi-drug resistant tuberculosis (MDR) requiring longer therapy with more drugs. Malaria, caused by one of five species of a parasite that are carried by mosquitos, has become increasingly difficult to treat because of this issue. Malaria cases in the United States have been relatively rare, about 1,200 per year while annually there are 300 million cases and one million deaths from the disease elsewhere in the world.
Most US cases have occurred in those who travel to sub-Saharan Africa, India, or Southeast Asia; That is likely to change as the expected average temperature increase of 0.4 degrees Celcius over the next eight years will likely increase our mosquito population by up to 30%, including the one mosquito species that carries the Plasmodium falciparum, the most deadly type that I've only seen when I was serving at the Air Force Regional Medical Center located on Clark AFB in the Philippines.
A recent online copy of The New York Times has an article titled, "Pressure Grows to Created Drugs for Superbugs." Health and Human Services (HHS) is going to pay $40 million to a pharmaceutical company to develop new antibiotics to combat drug resistance; they are concerned about biological agents that terrorists may utilize to cause widespread death.
But in the meantime, tens of thousands of our citizens die from inceptions, mostly hospital-acquired and caused by the current generation of antibiotic resistant germs. The FDA's director of the Center for Drug Evaluation and research was quoted as saying, "We are facing a huge crisis worldwide not having an antibiotic pipeline... but what is worse is the thought of where we will be five to 10 years from now."
A move to fast-track approval of new anti-infective drugs is being hotly debated. The Infectious Disease Society of America would support their labeling for use on only the very sickest patients.
Others are concerned that these restrictions are insufficient; that the new medicines will be used for those less-than critically ill without our knowing how the antibiotics will perform and what their advise effects may be. One director of the infectious disease society said, "The last thing we want is for a new drug to be overused."
The next twenty to fifty years will be a critical time for the germs versus humans war.